By Lane Lenard, Ph.D.
 Urinary incontinence (UI) is a common disorder affecting at least 51 million people in the United States. Women are especially prone to UI – half of all women experience incontinence at some point in their lives, and for one in three, UI is a chronic condition. Incontinence is more prevalent among adults 60 years of age or older, affecting more than 15 percent of older adults who live at home, and up to 60 percent of people living in nursing homes. UI is one of the most common reasons for nursing home admission.
Urinary incontinence (UI) is a common disorder affecting at least 51 million people in the United States. Women are especially prone to UI – half of all women experience incontinence at some point in their lives, and for one in three, UI is a chronic condition. Incontinence is more prevalent among adults 60 years of age or older, affecting more than 15 percent of older adults who live at home, and up to 60 percent of people living in nursing homes. UI is one of the most common reasons for nursing home admission.
For many, the fear of losing control of such a basic bodily function is so stressful and distressing that fewer than half of those with incontinence feel comfortable discussing their symptoms with their doctor. Commenting on the severity of the problem, Dr. Seth Landefeld, geriatrics chief at the University of California, San Francisco, notes that, “We as a society need to get over our discomfort with this subject so that incontinence sufferers receive the compassion, acceptance, and care they need, and our aging population can take steps to prevent incontinence in the future.”
Women’s Secret Burden
While the statistics are striking, the toll incontinence takes on one’s quality of life can be devastating, especially for women. Initially, most women find that occasional leaks can be controlled by wearing specially designed pads. But as the condition worsens, larger pads, or pads with greater absorptive capacity, may be needed. And while pads are usually effective for controlling leakage they do little to alleviate the other ways that UI influences daily life.
For example, one must learn to be constantly “tuned in” to the slightest signal from the bladder that it is time to go. And even simple tasks, such as going out to the store, require advance planning to pinpoint the location of nearby bathrooms for frequent emergency visits when the bladder is too full. Women also need to be particularly cautious about standing up quickly after sitting, especially when consuming liquids, and dark clothes are the preferred fashion choice because they are less prone to reveal dampness.
For many women, despite all the restrictions that UI imposes on their lives, the social stigma imposed by the disorder is the most overwhelming aspect of incontinence. The dread of a small cough or laugh triggering a “leak” during a social or business situation robs women of the pleasure such events offer and causes many women to limit or even avoid social activities all together. And at home, women may begin to avoid sex with their partners out of fear of embarrassment during intercourse. If not addressed, incontinence can lead to isolation and inactivity, allowing depression to take over and sadly, leading to further isolation and deepening depression.
Types of Urinary Incontinence
While UI in men is primarily associated with prostate enlargement, women are affected by three major types of urinary incontinence: stress incontinence, urge incontinence, and overactive bladder. Many women have a combination of two or three of these, which is referred to as mixed incontinence. To understand the types of incontinence, and their underlying causes, we must briefly review the bladder and its muscles.
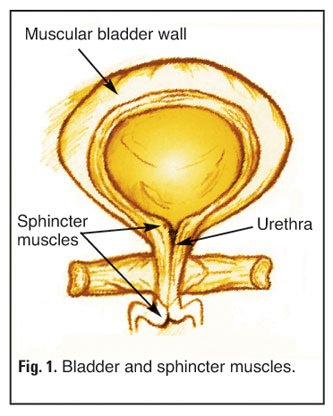
The balloon-like bladder (Fig. 1) stores urine after delivery from the kidneys (not shown). The bladder is surrounded by a muscular wall. Normally, leakage from the bladder is prevented by sphincter muscles that keep the urethra – the tube that carries urine from the bladder out of the body – shut at either end. When we urinate, the bladder muscle contracts and the two sphincters relax, so that urine is squeezed out through the urethra. Incontinence occurs when the bladder muscle contracts suddenly – and inappropriately – and/or the sphincters are too weak to hold back the urine.
- Stress Incontinence is typically associated with coughing, laughing, exercise, or other movements that put pressure on the bladder. It commonly occurs as a result of physical changes following pregnancy, childbirth, and menopause that weaken the sphincters.
- Urge Incontinence occurs if you suddenly and uncontrollably lose urine for no apparent reason after feeling the need or urge to urinate. Typically, you feel a slight urge to urinate, and suddenly, possibly before you can get to the toilet, you lose control. Inappropriate contractions, or spasms, of the bladder muscle, even when there is only a small amount of urine in the bladder, are a common cause of urge incontinence. These spasms may be triggered by abnormal nerve signals.
- Overactive Bladder is a result of the bladder muscle squeezing at the wrong time without warning and too frequently. Symptoms include high urinary frequency (eight or more times per day and two or more times per night); urinary urgency (the sudden, strong need to urinate immediately); and urge incontinence.
- Overflow Incontinence occurs primarily in older men with prostate enlargement. The enlarged prostate squeezes the urethra, which prevents the bladder from emptying completely. Overflow incontinence usually takes the form of dribbling, resulting in an inability to urinate voluntarily, overdistending the bladder and reducing the flow of urine.
Controlling Incontinence
Incidence of incontinence tends to increase with age for a variety of reasons, including: a reduction in the capacity of the bladder, leading to greater frequency of urination; weakening of urinary sphincter muscles; and decreased bladder muscle tone. In men, the prostate often enlarges with age.
Women with UI learn to cut down on, or even eliminate certain foods and beverages that act as diuretics to stimulate urination, such as coffee, tea, or anything else with caffeine; alcohol; citrus fruits and juices; and spicy or acidic foods. Certain drugs, especially those prescribed for high blood pressure or edema (swelling), act as powerful diuretics and should be avoided if possible (in consultation with a doctor).
Of course, staying properly hydrated can become another problem that requires attention and a delicate balance. While taking steps to avoid excess intake of liquids of any kind, women also have to avoid becoming dehydrated, which can lead to constipation, among other serious conditions. Exercise, vital for maintaining health in later years, can also trigger additional loss of urine, further complicating life for those with UI.
While special exercises known as Kegels can be helpful in reducing certain types of UI, they require dedication and patience, since it can take several weeks before they manifest any benefit.
Incontinence Drugs
Pharmaceutical companies have developed a number of drugs designed to ease the symptoms of UI, although none are completely effective, and disturbing side effects are often a problem.
- Anticholinergics: Muscle tone, including the muscles that control bladder contractions, is largely under the control of the neurotransmitter acetylcholine (ACh). Thus, drugs that interfere with the actions of ACh – known as anticholinergics – can sometimes be of help, especially for urge incontinence and overactive bladder because they relax the bladder muscle. According to drug company research, these drugs inhibit involuntary bladder contractions, increase bladder capacity, and delay the initial urge to void. Marketed anticholinergic drugs indicated for urge incontinence include Ditropan® and Oxytrol® (oxybutynin); Detrol® (tolterodine); and Levabid® and Cystospaz® (hyoscyamine).
- Antispasmodics: These drugs, which also have anticholinergic properties, are designed to help relax the bladder muscle in patients with urge incontinence and also sometimes help with overactive bladder. The most common antispasmodics are Urispas® (flavoxate) and Bentyl® (dicyclomine). Although these drugs have been used for years, their effectiveness is questionable. The newest antispasmodic drugs, Sanctura® (trospium chloride) and Enablex® (darifenacin), also work by interfering with the actions of ACh.
- Alpha-adrenergic agonists: Unlike anticholinergic drugs, which are designed to weaken bladder muscles, alpha-adrenergic agonists are intended to strengthen the smooth muscle that controls the sphincters at either end of the urethra. The most common drugs in this class include ephedrine and pseudoephedrine, which are commonly found in over-the-counter decongestants and appetite suppressants. Although these drugs may be helpful for some women with mild stress incontinence, their side effects – agitation, insomnia, and anxiety – can be disturbing. They are also not suitable for people with heart disease, high blood pressure, glaucoma, diabetes, or hyperthyroidism.
Problems with ACh Drugs
The major problem with drugs that affect ACh activity is that this neurotransmitter has actions, not just in the bladder muscle, but all over the body, in nearly all muscles, as well as in the brain. Common side effects include dry mouth, dry eyes, headache, constipation, rapid heart rate, glaucoma, muscle weakness, dizziness, drowsiness, and restlessness.
A recent study by a US Navy neurologist confirmed that these drugs can cause serious mental problems in some older people, including loss of memory and hallucinations. At a recent meeting of the American Academy of Neurology, neurologist Dr. Jack Tsao described one 73-year-old woman who began hallucinating conversations with dead relatives shortly after starting on a common incontinence drug. The hallucinations ceased when she stopped taking the drug.
Dr. Tsao and colleagues then systematically evaluated 870 older Catholic priests, nuns, and brothers for nearly 8 years. Almost 80 percent of the participants were taking anticholinergic drugs, including the incontinence drugs Ditropan and Detrol, for high blood pressure, asthma, Parkinson’s disease, as well as UI. The incontinence drugs were among the most potent and most frequently taken of all the anticholinergics in the study.
They found that those who were taking the drugs had a 50 percent faster rate of cognitive decline than those who were not taking them. “It may be better to use diapers and be able to think clearly than the other way around,” noted Dr. Tsao.
Natural Support for Enhanced Bladder Control
FloControl® is an advanced herbal formula designed to safely support urinary tract health and restore control over normal bladder functions. The proprietary consists of a proprietary blend of traditional Chinese herbs long recognized for their ability to promote healthy bladder function, including:
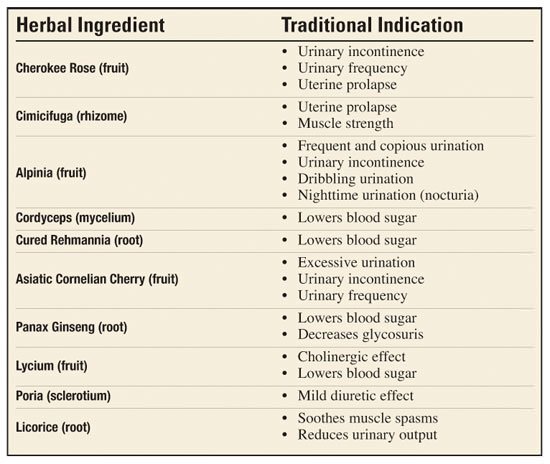
By restoring bladder strength and muscle tone, FloControl reduces both stress and urge incontinence. And in men, FloControl has been shown to enhance muscle tone to reduce dribbling and restore normal urinary performance.
References
1. D Bensky and A Gamble, Chinese Herbal Medicine – Materia Medica, Eastland Press, Seattle, Washington
2. Li SP, Zhang GH, Zeng Q, et al. Hypoglycemic activity of polysaccharide, with antioxidation, isolated from cultured Cordyceps mycelia. Phytomedicine. 2006 Jun;13(6):428-33. Epub 2005 Sep 19.
3. Zhang R, Zhou J, Jia Z, Zhang Y, Gu G. Hypoglycemic effect of Rehmannia glutinosa oligosaccharide in hyperglycemic and alloxan-induced diabetic rats and its mechanism. J Ethnopharmacol. 2004 Jan;90(1):39-43.
4. Yamabe N, Kang KS, Goto E, Tanaka T, Yokozawa T. Beneficial effect of Corni Fructus, a constituent of Hachimi-jio-gan, on advanced glycation end-product-mediated renal injury in Streptozotocin-treated diabetic rats. Biol Pharm Bull. 2007 Mar;30(3):520-6.
5. Lee WK, Kao ST, Liu IM, Cheng JT. Increase of insulin secretion by ginsenoside Rh2 to lower plasma glucose in Wistar rats. Clin Exp Pharmacol Physiol. 2006 Jan-Feb;33(1-2):27-32.
6. Luo Q, Yan J, Zhang S. Isolation and purification of Lycium barbarum polysaccharides and its anti-fatigue effect. Wei Sheng Yan Jiu. 2000 Mar 30;29(2):115-7.
7. Luo Q, Cai Y, Yan J, Sun M, Corke H. Hypoglycemic and hypolipidemic effects and antioxidant activity of fruit extracts from Lycium barbarum. Life Sci. 2004 Nov 26;76(2):137-49.












