by Jim English
Periodontal disease is a chronic inflammatory disorder that causes gum tissues to pull away from the teeth, allowing bacteria to accumulate and triggering an inflammatory reaction that leads to the loss of bone tissues and teeth. In addition to the loss of teeth, researchers have linked the onset of periodontal disease with other chronic inflammatory disorders, including diabetes, cardiovascular disease, prostatitis and rheumatoid arthritis.
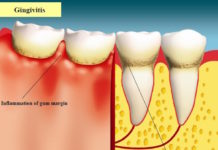
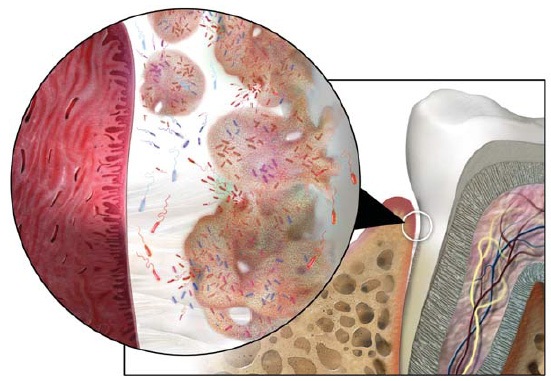 Gum disease begins when bacteria gather to form a “biofilm” that coats tooth surfaces at or below the gum line. These bacteria emit toxins that cause the body to mount an inflammatory response that, in turn, begins to eat away at gum tissues, leading to gingivitis. Eventually, if the source of inflammation is not brought under control, the process can result in the destruction of supportive bone structures (alveolar bone) that play a critical role in anchoring teeth firmly in place. As these retaining tissues break down, once-firm teeth become loose, leading to increasing inflammation, loss of bone and eventually requiring extraction.
Gum disease begins when bacteria gather to form a “biofilm” that coats tooth surfaces at or below the gum line. These bacteria emit toxins that cause the body to mount an inflammatory response that, in turn, begins to eat away at gum tissues, leading to gingivitis. Eventually, if the source of inflammation is not brought under control, the process can result in the destruction of supportive bone structures (alveolar bone) that play a critical role in anchoring teeth firmly in place. As these retaining tissues break down, once-firm teeth become loose, leading to increasing inflammation, loss of bone and eventually requiring extraction.
Gum Health and Periodontitis
While periodontitis is recognized as the most common form of chronic infection and inflammation in humans, the number of people in the United States afflicted with periodontitis turns out to be significantly higher than was originally believed. In a recent National Health and Nutrition Examination Survey (NHANES) study, a full-mouth, comprehensive periodontal examination of over 450 adults over the age of 35 was compared with the results of earlier studies that relied on only a partial-mouth periodontal examination. The recent study shows that the previous partial-mouth study methodology may have underestimated the true incidence of periodontal disease by up to 50 percent.(1)
According to Samuel Low, DDS, MS, president of the American Academy of Periodontology, “This study shows that periodontal disease is a bigger problem than we all thought. It is a call to action for anyone who cares about his or her oral health. Given what we know about the relationship between gum disease and other diseases, taking care of your oral health isn’t just about a pretty smile. It has bigger implications for overall health, and is therefore a more significant public health problem.”
How ‘Jailbreaking’ Bacteria can Trigger Heart Disease
A growing body of research now links gum disease with the onset of heart disease, caused when plaque-causing bacteria from the mouth enter into the bloodstream and increase the risk of heart attack. According to Professor Howard Jenkinson of the University of Bristol, England, oral bacteria can wreak havoc if they are not kept in check by regular brushing and flossing. “Poor dental hygiene can lead to bleeding gums, providing bacteria with an escape route into the bloodstream, where they can initiate blood clots leading to heart disease,” he said.(2)
Streptococcus bacteria commonly live in the mouth, confined within communities termed “biofilms” that are responsible for causing tooth plaque and gum disease. Researchers have now shown that once let loose in the bloodstream, Streptococcus bacteria can use a protein, called PadA, as a weapon to force platelets in the blood to bind together and form clots.
Inducing blood clots is a selfish trick used by bacteria, Jenkinson points out. “When the platelets clump together they completely encase the bacteria. This provides a protective cover not only from the immune system, but also from antibiotics that might be used to treat infection,” he said. “Unfortunately, as well as helping out the bacteria, platelet clumping can cause small blood clots, growths on the heart valves (endocarditis), or inflammation of blood vessels that can block the blood supply to the heart and brain.”
Professor Jenkinson said the research highlights a very important public health message. “People need to be aware that as well as keeping a check on their diet, blood pressure, cholesterol and fitness levels, they also need to maintain good dental hygiene to minimize their risk of heart problems.”
Periodontal Disease Linked to Prostatitis
In addition to contributing to development of heart disease, researchers from Case Western Reserve University School of Dental Medicine recently reported that initial results from a small sample shows that inflammation from gum disease and prostate problems just might be linked. In their paper, published in the official journal of the American Academy of Periodontology, the researchers described how they compared two unique markers for inflammation: Prostate-Specific Antigen (PSA), which is widely used to measure inflammation levels in prostate disease, and Clinical Attachment Level (CAL) of the gums and teeth, an indicator of periodontitis.
A PSA blood level of 4.0 ng/ml in the blood can be a sign of inflammation or malignancy, and patients with healthy prostate glands have lower than 4.0 ng/ml levels. A CAL number greater than 2.7 mm indicates periodontitis.
Like periodontitis, prostatitis also produces high inflammation levels. “Subjects with both high CAL levels and moderate to severe prostatitis have higher levels of PSA or inflammation,” stated Nabil Bissada, chair of the department of periodontics in the dental school. Bissada added that this might explain why PSA levels can be high in prostatitis, but sometimes cannot be explained by what is happening in the prostate glands. “It is something outside the prostate gland that is causing an inflammatory reaction,” he said. Because periodontitis has been linked to heart disease, diabetes and rheumatoid arthritis, the researchers felt a link might exist to prostate disease.
Thirty-five men from a sample of 150 patients qualified for their study, funded by the department of periodontology at the dental school. The participants were selected from patients with mild to severe prostatitis, who had undergone needle biopsies and were found to have inflammation and in some patients, malignancies.
The participants were divided into two groups: those with high PSA levels for moderate or severe prostatitis or a malignancy, and those with PSA levels below 4 ng/ml. All had not had dental work done for at least three months and were given an examination to measure the gum health. Looking at the results, the researchers from the dental school and the department of urology and the Institute of Pathology at the hospital found those with the most severe form of the prostatitis also showed signs for periodontitis.(3)
Polyunsaturated Fatty Acids may Reduce Periodontitis
In an article in the November issue of the Journal of the American Dietetic Association, researchers from Harvard Medical School and Harvard School of Public Health report that dietary intake of polyunsaturated fatty acids (PUFAs) like fish oil, known to have anti-inflammatory properties, shows promise for the effective treatment and prevention of periodontitis.
In a study involving over 9,000 adults, researchers found that omega-3 fatty acid intake, particularly docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA), were associated with reduced incidence of periodontitis. One of the study authors, Asghar Z. Naqvi commented, “To date, the treatment of periodontitis has primarily involved mechanical cleaning and local antibiotic application. Thus, a dietary therapy, if effective, might be a less expensive and safer method for the prevention and treatment of periodontitis. Given the evidence indicating a role for omega-3 fatty acids in other chronic inflammatory conditions, it is possible that treating periodontitis with omega-3 fatty acids could have the added benefit of preventing other chronic diseases associated with inflammation, including stroke as well.”
In their paper, the researchers reported an approximately 20 percent reduction in incidence of periodontitis in those consuming the highest amount of dietary DHA. The reduction correlated with EPA was smaller, while the correlation to LNA was not statistically significant. Foods that contain significant amounts of polyunsaturated fats include fatty fish like salmon, peanut butter and nuts.(4)
Summary
Given the increasing prevalence of periodontal disease and the growing body of research connecting periodontal health and systemic health, it is clearly essential to take steps to maintain healthy teeth and gums. According to Dr. Low, “Not only should you take good care of your periodontal health with daily tooth brushing and flossing, you should expect to get a comprehensive periodontal evaluation every year,” he advised. A dental professional, such as a periodontist, a specialist in the diagnosis, treatment and prevention of gum disease, will conduct the comprehensive exam to assess your periodontal disease status.
References
1. P. I. Eke, G. O. Thornton-Evans, L. Wei, W. S. Borgnakke, B. A. Dye. Accuracy of NHANES Periodontal Examination Protocols. Journal of Dental Research, 2010.
2. Society for General Microbiology (2010, September 5). ‘Jailbreak’ bacteria can trigger heart disease.
3. Joshi et al. Association Between Periodontal Disease and Prostate Specific Antigen Levels in Chronic Prostatitis Patients. Journal of Periodontology, 2010.
4. Asghar Z. Naqvi, Catherine Buettner, Russell S. Phillips, Roger B. Davis, Kenneth J. Mukamal. n-3 Fatty Acids and Periodontitis in US Adults. Journal of the American Dietetic Association, 2010; 110.













[…] Consume DHA supplements […]