By Jim English
Alzheimer’s Disease (AD) is a progressive degenerative disease that commonly appears after the age of 50. Alzheimer’s afflicts approximately 40 percent of all individuals over the age of 85, or almost 4 million people in the U.S. When symptoms occur before the age of 65 the disease is designated Presenile Dementia of the Alzheimer’s Type (PDAT). When symptoms occur after age 65 the syndrome is referred to as Senile Dementia of the Alzheimer’s Type (SDAT). Symptoms include a gradual yet inexorable loss of memory, mental performance, communication skills, abstract thinking and personality. Ultimately, Alzheimer’s ends in the death of the patient, with a mean life expectancy of 8 years.
As well as being a profound tragedy for afflicted individuals and their loved ones, the financial costs of caring for victims of the disease exceed $80 billion per year. The current trend towards longer life expectancy, combined with the increased incidence of senile dementia with age, means that cases of Alzheimer’s are increasing as the median age of the population grows, further underscoring the urgent need to find an effective treatment for this disorder.
Cholinergic Dysfunction
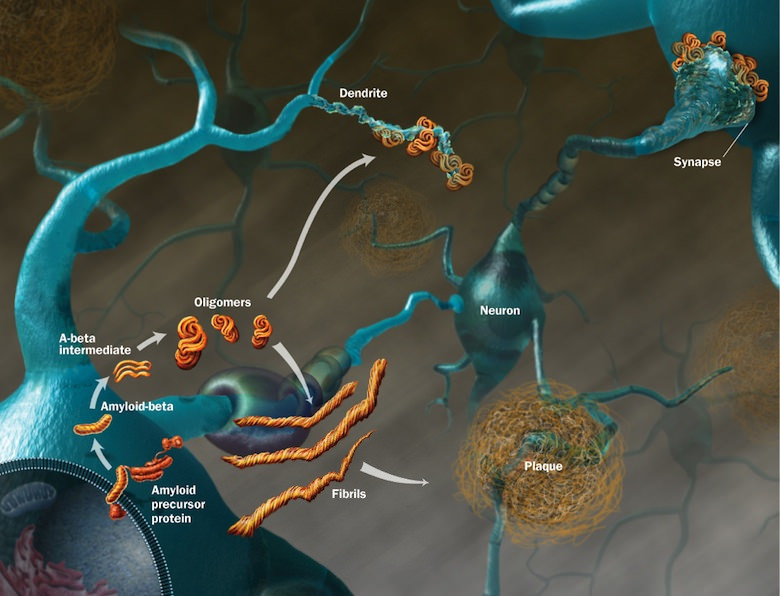
Alzheimer’s is characterized by the destruction of nerve cells in key areas of the brain devoted to mental functions. This results in tangles of nerve fibers and plaque formation of an abnormal, insoluble protein called amyloid. While there is a general reduction in the concentration of all neurotransmitting substances, a marked clinical feature of the disease is a dramatic decrease in the neurotransmitter acetylcholine.
Acetylcholine is a vital neurotransmitter with a fundamental role in memory. It is also necessary for proper intracellular communication between nerve cells. Research has shown that levels of acetylcholine are deficient in the brains of patients with Alzheimer’s disease.
Biopsy and postmortem studies have revealed a substantial loss of presynaptic cholinergic neurons in brains of patients with Alzheimer’s.1 What little acetylcholine that is still produced in the patient’s brain is quickly broken down by the brain enzyme, acetylcholinesterase (AChE), leading to a shortage of the neurotransmitter and contributing to loss of memory and other cognitive functions.
Two drugs approved for treating Alzheimer’s – Tacrine™ and Donepezil hydrochloride (Aricept™) – are moderately effective acetylcholinesterase inhibitors that work by interfering with the actions of AChE. Since acetylcholine is normally degraded and recycled by acetylcholinesterase, this approach counteracts any further reduction of already low levels of acetylcholine. By inhibiting the actions of AChE it is hoped that the small amounts of acetylcholine still being produced will persist longer within the synaptic cleft and lead to improvements in memory and cognitive abilities.
While both drugs are effective acetylcholinesterase inhibitors, they suffer from a number of drawbacks. First, they are available only by prescription; second, they are expensive, costing between $100 to $240 per month; and third, both drugs can cause debilitating side effects including liver toxicity (Tacrine), and nausea and diarrhea (Donepezil). (1)
Huperzine A
Huperzine A is a natural compound derived from an ancient Chinese remedy, Qian Ceng Ta. This traditional herbal medicine was prepared from Huperzia serrata, a type of clubmoss that grows on the ground in damp forests and rock crevices. Brewed as an herbal tea, Qian Ceng Ta has been used in China for centuries as a diuretic and to treat fever, inflammation and irregular menstruation.
In the late 1980’s, researchers in China discovered that a purified alkaloid extracted from Huperzia – Huperzine A – was a potent, reversible inhibitor of acetylcholinesterase (AChE). Huperzine A was shown to readily cross the blood-brain barrier to prevent acetylcholinesterase (AChE) from destroying acetylcholine.
Molecular Monkey Wrench
A study at the Weizmann Institute in Israel uncovered how Huperzine A (Hup-A) works to block acetylcholinesterase. (2) Scientists had previously learned that AChE inhibitors such as tacrine and donepezil worked by sliding into the AChE molecule to “jam up” its molecular machinery and impair its ability to degrade acetylcholine.
By imaging a 3-dimensional structure of the AChE molecule, the researchers were able to peer into the complex folded protein structure to discover a deep chasm, called the active-site gorge. The scientists determined that the active-site gorge acts as a guide to funnel acetylcholine into the interior of the enzyme where it is cut apart prior to recycling.
This study revealed that Huperzine A has a strong specificity for AChE, and is exceptionally well-suited to its new role, fitting into the active sites of acetylcholinesterase much like a key slipping into a lock. “Hup-A appears to bind more tightly and specifically to acetylcholinesterase than the other AChE inhibitors,” crystallographer Prof. Joel Sussman, one of the authors of the study said. “It is as if this natural substance was ingeniously designed to fit into the exact spot in AChE where it will do the most good.”
Clinical Studies
Double-blind, placebo-controlled clinical trials in China demonstrated that patients suffering from Alzheimer’s and various other memory disorders gain significant benefit, both in terms of memory and life quality. Xu et al. conducted a placebo-controlled, double-blind study in which subjects with AD were given 200 mcg/day Huperzine A or a placebo for 8 weeks. Statistically significant improvements were noted in 58 percent of the treated group with respect to cognitive function and their ability to retrieve past memories. (3)
A second study conducted by researchers t the Department of Pharmacology, Zhejiang Academy of Medical Sciences, examined the effects of Huperzine A on six volunteers. They concluded that Hup-A had a high rate of absorption and distribution in the body, and was free of adverse side effects. (4)
Another study conducted by the same researchers focused on the efficacy of Huperzine A on memory, cognition, and behavior in Alzheimer’s disease. This multicenter, double-blind, placebo controlled study found that about 58 percent (29 out of 50) of patients treated with Hup-A showed improvements in their memory, cognition, and behavioral functions. No side effects were found. The researchers concluded that “Hup-A is a promising drug for symptomatic treatment of Alzheimer’s disease.” (4)
In a related paper, noted neurologist, Alan A. Mazurek, M.D., reported on the results of an office-based trial studying the safety and efficacy of Huperzine A as a treatment for Alzheimer’s disease. Mazurek evaluated the safety and efficacy of Hup-A in an open-label trial involving 29 patients with mild to moderate AD. (5) Twenty-two patients (75.9 percent) completed the three-month study. Only two patients reported adverse effects, one being an apparently unrelated hemorrhagic infarct that resolved without treatment. No gastrointestinal side effects, nausea, diarrhea, cardiac effects or headache were reported. Status Examinations’ (SMMSE) improvement of one point or greater was seen at one, two and three months. Mazurek reported that improvements appeared to be dose related, with those on the higher dosages exhibiting the greatest improvement. Wrote Mazurek, “Huperzine A appears to be safe, well-tolerated, and effective in the symptomatic treatment of AD.”
Other Benefits
In addition to its activity as an AChE inhibitor, ongoing research suggests that Hup-A has a wider role to play in supporting neuroprotective functions. Researchers recently discovered that Hup-A inhibits glutamate-induced cytotoxicity, protecting neonatal hippocampal and cerebellar neuronal cells in culture from death caused by the amino acid glutamate. In addition to protecting from glutamate-induced cytotoxicity, researchers were also surprised to learn that Huperzine A promotes new dendrite outgrowth of neuronal cultures.
Potential Protection for Chemical Warfare
Researchers at the Walter Reed Army Institute of Research in Washington D.C. have conducted studies into Huperzine’s potential role as a pretreatment drug to protect against chemical warfare nerve agent poisoning. In one study, Hup-A was found to be twice as effective in protecting mice against the lethal effects of the nerve agent soman when compared to physostigmine. (6) Hup-A’s effects lasted for six hours compared to only 90 minutes for physostigmine, providing further evidence for the slow clearance of Huperzine from the body.
Summary
Huperzine A has a wide margin of safety. Toxicology studies show Huperzine A to be non-toxic even when administered at 50-100 times the human therapeutic dose with no remarkable side effects. Clinical research has shown that Huperzine A is superior to other cholinesterase inhibitors such as tacrine and donepezil. Huperzine A is rapidly absorbed when taken orally, and possesses a very slow rate of dissociation from the enzyme and a longer duration of action
Huperzine A has been shown to be effective in inhibiting the actions of AChE to increase acetylcholine concentrations and alleviate some of the symptoms associated with acetylcholine deficiencies. Significant effects have been noted in patients both in terms of their life quality and their ability to retrieve past memories. These findings suggest that Hup-A is a unique and exciting supplement for supporting memory in the healthy aging human.
References
1. Watkins PB, Zimmerman HJ, Knapp MJ. Hepatotoxic effects of tacrine administration in patients with Alzheimer’s disease. JAMA 1994 Apr 6; 271:992-8
2. Raves ML, Harel M, Pang YP, Silman I, Kozikowski AP, Sussman JL. Structure of acetylcholinesterase complexed with the nootropic alkaloid, (-)-huperzine A. Nat Struct Biol 1997 Jan;4(1):57-63.
3. Xu SS; Gao ZX; Weng Z; Du ZM; Xu WA; Yang JS; Zhang ML; Tong ZH; Fang YS;Chai XS; et al, Efficacy of tablet huperzine-A on memory’ cognition’ and behavior in Alzheimer`s disease. Chung Kuo Yao Li, Hsueh Pao16:391-5, 1995.
4. (Qian BC, Wang M, Zhou ZF, Chen K, Zhou RR, Chen GS. Pharmacokinetics of tablet huperzine A in six volunteers. Chung Kuo Yao Li Hsueh Pao 1995 Sep;16(5):396-8)
5. Mazurek, A. An open label trial of Huperzine A in the treatment of Alzheimer’s disease. Alternative Therapies, March 1999. Vol. 5, No. 2:97.
6. Saxena A, Qian N, Kovach IM, Kozikowski AP, Pang YP, Vellom DC, Radic Z, Quinn D, Taylor P, Doctor BP. Identification of amino acid residues involved in the binding of Huperzine A to cholinesterases. Protein Sci 1994 Oct;3(10):1770-8.












[…] It leads to better memory development, faster recall and lasting recollection. Fundamentally, Huperzine A supplement enhances the ability of your brain’s nerve cells to link quickly, and communicate better and faster with each other. It further leads to superior cognitive ability. […]